Chronic pain is hard. Especially when it’s one of several conditions or symptoms you’re juggling through the day. You aren’t alone – up to 50% of the UK adult population experience chronic pain, and according to UK government data if you’re living with a disability you’re twice as likely to be affected by long term pain.,,
Dr. Ashish Shetty is a Consultant in Pain Medicine at the National Hospital for Neurology and Neurosurgery, University College London Hospitals and NuroKor’s Chief Medical Officer. He explains why living with pain can be so difficult and how if you are one of the 28 million people in the UK affected, you can stop pain ruining your day.
Despite being common, chronic pain is very personal – it affects everyone differently. Whilst some have constant pain, others are prone to flare-ups. Both drastically affect how you feel, both physically and mentally. It can impact your ability to work and interfere with the activities of daily living. Finding a solution to manage the pain isn’t always plain sailing either and many people feel that long-term, prescription pain relief is their only option, which can present problems of its own.
The good news is, there are other effective and sustainable solutions that are worth looking into; in the same way that everyone’s pain is very individual, so are the options. Although there is no magic fix-all solution, it’s often a combination that makes the most difference – it’s all about finding what works for you.
If you experience pain, here are five different things you can explore and try incorporating into your daily pain management strategy.
- Psychological support
When psychological support for pain management is suggested it can sometimes feel as if your pain and your experience aren’t being recognised. Pain is multifaceted and requires a multidisciplinary approach . It is important to remember that suggestion of psychological support is not to suggest that the source of your pain is psychological – in fact, it’s the opposite. Chronic pain has been shown to affect mental health. Being in pain can feel hopeless and a heavy burden to bear, so psychological support can go a long way to help you manage your pain symptoms.
Options can include counselling, cognitive behavioural therapy, relaxation or even medication.
- Trigger diaries (Pain diary)
For some people, their pain and flare-ups follow clear patterns, but for others it can feel like pain onsets for no apparent rhyme or reason – either way it can be incredibly disruptive to life. Maintaining a pain diary might help in identifying the triggers that influence the timings of flare- ups or even the severity of pain. Triggers can be as easy to identify as heavy exercise or disrupted sleep, to simple day-to-day activities like cooking, cleaning, watching TV, driving. Other triggers include stress, food, allergies, hormones or changes in the environment.

By identifying how potential triggers are influencing your pain, rather than whether or not it’s causing it, can help give insight into the best way to manage on a day-to-day and flare-up-to-flare-up basis. It could be that some of these triggers could cause flare-ups, but are not necessarily indicative of the source of the pain. You can also use this information to support conversations with your care teams, to help identify the best approach and care for you and pace your daily activity levels
3) Diet and Lifestyle changes
Understanding what makes your pain worse, or what makes your pain better, is helpful to understand and create a manageable plan for how to live day-to-day, and help to avoid flare-ups. A balanced diet and a healthy lifestyle is essential for the wellbeing of every individual. This becomes more important when one has chronic conditions.
4) Exercise and Hydrotherapy
Exercise is not always an option when you’re experiencing chronic pain. However, gentle exercise, within the parameters of what is comfortable and doesn’t exacerbate symptoms can help to release endorphins and relax the body.
It doesn’t need to be strenuous and you don’t even need to break a sweat – something as simple as chair yoga, seated pilates, or a gentle stretching routine could help get your body loving a little. Any exercise that doesn’t exacerbate the problem and helps maintain a range of motion is a net positive.
For lots of people water can feel calming – sometimes even just being near water can help them to relax. Physiologically, being able to get into the water is even better as it can not only ease the pressure on your body but can help to soothe your skin and muscles.
Simply floating in water will get your body moving in a safe, comfortable and pain-free way. It has also been proved to increase endorphins and aid in relaxation, for the treatment of everything from chronic pain to PTSD.,
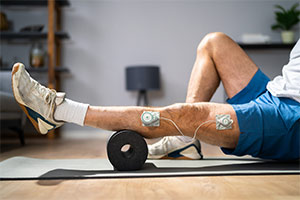
5) Bioelectronics
Whilst various pain devices have been around for a while and have some limited use, personalised, targeted technology like NuroKor Lifetech that uses peripheral nerve stimulation and microcurrent stimulation technologies, are being increasingly recommended and endorsed by healthcare professionals and clinical experts as an effective way of managing pain and recovery from injury.
The use of electrical stimuli to manage pain is probably the oldest treatment known to humans. The Greeks used torpedo fish to deliver electrical current to treat headaches in 47 AD.
Microcurrent uses electrical currents that are so small that you barely feel them. The current is utilized by your body’s cells to support recovery and benefit joints and soft tissues such as the muscles, tendons and ligaments. External stimulation NuroKor devices use electricity in a controlled fashion using special algorithms to interrupt the pain signals traveling to the brain via the nervous system.
These handheld devices are safe to use on multiple parts of the body, and have numerous programmes, tailored specifically to the type of pain and location, to provide instant and enduring pain relief. In a recent patient survey, 86% reported pain relief for at least six hours, with some reporting sustained relief one week and even one month later. A further 91% of patients also experienced a significant reduction or total elimination of pain and the same number reduced or eliminated the need for pain medication.